I know the specific, sharp terror that grips your heart when your child’s breathing sounds just a little too fast, or when a common cold suddenly transforms into a deep, rattling cough that seems to shake their entire small frame. As a parent, I have sat through those long nights, watching every rise and fall of a chest, wondering if we are headed for an emergency room visit. Pneumonia is a heavy word that carries a lot of fear, but understanding the clinical reality of this lung infection is the first step in moving from panic to purposeful care.
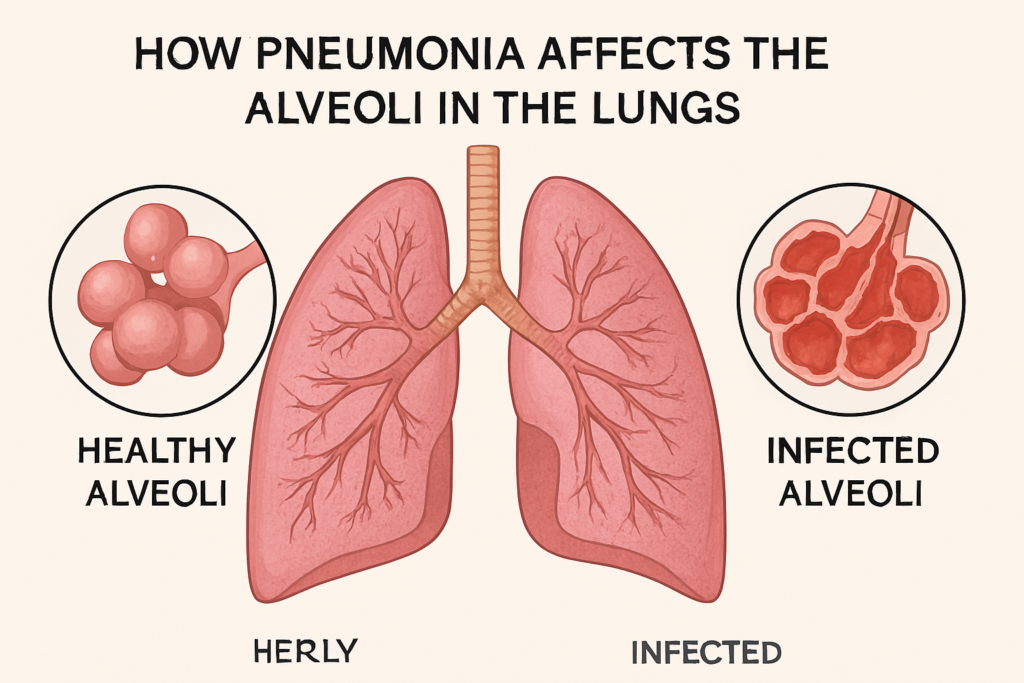
Pneumonia is an infection that inflames the air sacs in one or both of your lungs. These tiny sacs, known as alveoli, are the site where oxygen enters your blood. When pneumonia strikes, these sacs fill with fluid or pus, which makes it difficult to breathe and triggers symptoms like fever, chills, and a cough with phlegm. It can range in seriousness from a mild illness that feels like a stubborn cold to a life-threatening condition, particularly for infants, seniors over age 65, and those with underlying health problems.
I have seen how this illness impacts families, and I believe that being informed is your greatest defense. In this guide, I will walk you through the types of pneumonia, how to spot the signs in different age groups, the road to recovery, and how to manage the intense health anxiety that often follows such a diagnosis.
Understanding the Cause – Why Pneumonia Happens
I find that many parents are surprised to learn that pneumonia is not caused by just one type of germ. It is a condition that various “invaders” can trigger when they overpower your body’s natural defenses.
Bacterial Pneumonia This is often the most serious form of the infection. In the United States, the most common cause is the bacterium Streptococcus pneumoniae. I have seen bacterial pneumonia strike suddenly, or it may develop after a child has already been weakened by a cold or the flu. It often causes a high fever – sometimes up to 105 degrees Fahrenheit – and a cough that produces thick, yellowish-greenish, or even blood-tinged sputum.
Viral Pneumonia Viruses cause the majority of pneumonia cases in school-aged children. These are the same viruses responsible for the flu, COVID-19, and RSV. Symptoms of viral pneumonia usually develop over several days and can feel similar to the flu at first, with a dry cough, headache, and muscle pain. While often milder, viral pneumonia can still become severe and may pave the way for a secondary bacterial infection.
Walking Pneumonia You might have heard the term “walking pneumonia.” This is a milder form of the illness caused by bacteria-like organisms called Mycoplasma pneumoniae. I call it this because the symptoms are typically not severe enough to require bed rest, but they can linger with a stubborn, nagging cough.
Fungal Pneumonia This type is less common and primarily affects people with chronic health problems or weakened immune systems. These fungi are often found in soil or bird droppings.
Identifying Symptoms Across Different Ages
In my time studying family wellness, I have learned that pneumonia is a master of disguise. It does not look the same in a toddler as it does in a grandparent.
The Signs in Infants and Newborns Babies are the most vulnerable because they cannot tell us what hurts. They may not even have a cough at all. I tell parents to watch for these “silent” signals:
- Appearing restless, fussy, or unusually tired and limp.
- Rapid breathing or a “grunting” sound with every breath.
- Pale skin and fewer wet diapers than usual.
- Vomiting or difficulty feeding.
The Symptoms in Children and Adults For older children and healthy adults, the body usually sounds a louder alarm. Look for:
- A persistent cough that produces greenish, yellow, or bloody mucus.
- Sharp chest pain that feels worse when you take a deep breath or cough.
- Shaking chills, sweating, and a high fever.
- Shortness of breath or rapid, shallow breathing.
The Shift in Seniors and the Immunocompromised Adults over age 65 may experience pneumonia differently. Instead of a high fever, they might actually have a lower-than-normal body temperature. I have also noted that a sudden change in mental awareness—such as confusion or feeling less alert—is a very common sign in seniors.
The Path to a Professional Diagnosis
When I suspect pneumonia, I do not wait. Early medical intervention is crucial. Your healthcare provider will use several tools to solve the mystery of what is happening in the lungs.
Clinical Examination The doctor will start by listening to your lungs with a stethoscope. I have heard doctors describe the sounds of pneumonia as crackling, bubbling, or rumbling during inhalation. They will also check your appearance and vital signs, including your heart rate and breathing pattern.
Diagnostic Testing To confirm the diagnosis and determine the cause, several tests may be ordered:
- Chest X-ray: This is the primary way to see the location and extent of inflammation in the lungs.
- Pulse Oximetry: A small sensor is clipped to your finger to measure the oxygen levels in your blood.
- Blood Tests: These help identify if the infection is caused by bacteria or a virus.
- Sputum Test: A sample of mucus from a deep cough is analyzed in a lab.
In more serious or hospitalized cases, a CT scan or a bronchoscopy might be necessary to get a closer look at the airways.
“A timely diagnosis does more than just start treatment; it provides a roadmap that turns a scary unknown into a manageable plan”.

Masterful Recovery and Home Care
Healing from pneumonia is a slow process that requires patience. I have seen many people try to rush back to work or school, only to find themselves completely exhausted a few days later.
Medical Treatment Strategies The treatment depends entirely on the cause:
- Bacterial: Doctors prescribe antibiotics. It is vital that you finish the entire course, even if you feel better after two days, to prevent the infection from returning.
- Viral: Antibiotics do not work against viruses. Instead, you might receive antiviral medication if the infection is caught early, but the primary focus is on managing symptoms while the body fights back.
- Fungal: These cases require specific antifungal medications.
Supportive Care at Home I recommend focusing on these four pillars of recovery:
- Hydration: Drink plenty of fluids to help thin the mucus in your lungs so you can cough it up more easily.
- Rest: Sleep is when your body does its best repair work. Get plenty of it.
- Fever Control: Use acetaminophen or ibuprofen as directed for comfort.
- Important: Never give aspirin to children or teens due to the risk of Reye syndrome.
- Breathing Comfort: A humidifier or a steamy shower can help loosen chest congestion.
Navigating the Mental Toll and Health Anxiety
We must talk about the emotional impact of this illness. I have seen parents who, after a child’s bout with pneumonia, find themselves catastrophizing every future sniffle or cough. This health anxiety is a natural response to seeing a loved one struggle to breathe.
I want you to know that it is normal to feel “on high alert”. One parent shared that they immediately think an ER visit is around the corner whenever their kids get sick. To manage this, I suggest focusing on the clinical facts: fever is actually the body’s way of eliminating “intruders” and pathogens.
I also find inspiration in the stories of those who have faced even more severe challenges. One person who survived Stage 4 lung cancer and pneumonia noted that facing such a trial put their old issues into perspective and helped them find a strength they never knew they had. While the anxiety is real, you can use this experience to build resilience and a more positive mindset.
Strengthening Your Family’s Defenses
I believe that prevention is the most powerful tool in your wellness kit. You can take concrete steps to reduce your family’s risk of developing pneumonia.
The Power of Vaccination Vaccines are your first line of defense. I recommend staying up to date with:
- Pneumococcal vaccines, which protect specifically against pneumonia bacteria.
- Annual flu shots, as the flu is a common precursor to pneumonia.
- COVID-19 and RSV vaccinations, which prevent primary infections that can lead to lung inflammation.
Lifestyle and Hygiene I have seen how lifestyle choices directly impact lung health. Smoking damages your lungs’ natural defenses against bacteria and viruses. I have spoken with many people who used a bout of pneumonia as the final catalyst to quit smoking after years of addiction. They found that once they stopped, they felt more energetic and capable of breathing than they had in a decade.
I also recommend practicing good hygiene, such as regular handwashing, and keeping your immune system strong through a healthy diet, regular exercise, and enough sleep.
CONCLUSION: A Future of Clear Breathin
Walking the path of recovery from pneumonia is a journey of patience and resilience. I have seen how this illness can shake your confidence, but I have also seen how it can be a turning point for a healthier, more intentional life. Whether you are currently managing an infection or looking to protect your family’s future, remember that you are not alone in this.
Focus on the small victories—the first day the fever stays down, the first night of restful sleep, or the moment your child asks to go outside and play again. You are doing the vital work of caring for your family’s health. With the right medical guidance, a vigilant heart, and a focus on recovery, you will navigate this challenge and find your way back to a life of wellness and clear, deep breaths.
FAQ
Is pneumonia contagious?
Pneumonia itself is not generally contagious, but the viruses and bacteria that cause it are. You can spread the germs through coughs, sneezes, or sharing utensils, which might then lead to pneumonia in another person. For the latest U.S. public health guidelines, consult the CDC.
Can you have pneumonia without a fever?
Yes. This is most common in infants, seniors over 65, and people with weakened immune systems. You should monitor for other signs like rapid breathing or confusion instead of relying solely on a thermometer.
When should I go to the Emergency Room?
I advise seeking emergency care if you or your child struggle to breathe while sitting still, have bluish lips or fingernails, experience severe chest pain, or show sudden signs of confusion.
How long does the fatigue last after recovery?
While bacterial pneumonia often improves in 1-2 weeks with treatment, the fatigue and cough can linger for several weeks or even a month.
