I have spent years observing how respiratory health impacts families, and I know that few things are as concerning as a deep, rattling cough. Pneumonia is a serious infection that causes the tiny air sacs in your lungs, known as alveoli, to become inflamed. When this happens, these air sacs may fill with fluid or pus, making it difficult for you to breathe and for oxygen to reach your bloodstream. I believe that understanding the specific causes of pneumonia is the most important step you can take toward protecting your loved ones and managing recovery effectively.
Most of the time, your body is incredibly efficient at filtering germs out of the air you breathe. However, certain invaders can overpower your immune system, especially if your defenses are already low. Whether the culprit is a bacterium, a virus, or a fungus, the biological reaction is often similar: your immune system launches an attack, leading to the inflammation and fluid buildup that define this condition.
The Microbial Culprits Behind Lung Infections
When I discuss the causes of pneumonia, I find it helpful to categorize the pathogens into three main groups: bacteria, viruses, and fungi. Each of these invaders interacts with your lung tissue differently, but they all result in the same inflammatory response.
Bacterial Causes of Pneumonia Bacteria are the most common cause of pneumonia in adults. In the United States, the leading offender is Streptococcus pneumoniae, also known as pneumococcus. I have found that bacterial pneumonia can develop as a primary infection or as a secondary complication after you have had a cold or the flu.
There are also atypical bacteria, such as Mycoplasma pneumoniae, which usually cause a milder form of the illness often referred to as walking pneumonia. Other bacterial causes include Haemophilus influenzae, Chlamydia pneumoniae, and Legionella pneumophila, the latter of which causes Legionnaires’ disease.
Viral Causes of Pneumonia Viruses are the leading cause of pneumonia in children under the age of five. I often see viral pneumonia triggered by the flu (influenza) or the common cold (rhinovirus). Respiratory syncytial virus (RSV) is also a very common cause in young children.
More recently, SARS-CoV-2, the virus responsible for COVID-19, has become a significant cause of severe viral pneumonia. While viral pneumonia is often milder than bacterial versions, it can sometimes become very serious or lead to a secondary bacterial infection.
Fungal Causes of Pneumonia Fungal causes of pneumonia are less common but can be very dangerous for individuals with weakened immune systems. I have observed that fungi like Pneumocystis jirovecii often affect those who are immunocompromised. Some fungi are found in specific geographic locations, such as the soil in the Ohio and Mississippi River Valleys or bird droppings.
Beautiful Insight: It is important to remember that while the bacteria and viruses that lead to pneumonia are contagious, the pneumonia itself is a specific internal reaction. You can catch a virus from someone, but your body’s unique immune response determines if it develops into a lung infection.
Classifying Pneumonia by Environment and Origin
I have learned that medical professionals often classify pneumonia based on where the infection was acquired. This classification is vital because it helps me understand which germs are likely involved and how they might respond to treatment.
Community-Acquired Pneumonia (CAP) This is the most frequent type of pneumonia. It refers to infections caught in your daily life—at work, school, or in the grocery store. For example, if your child brings home an infection from school, it is categorized as community-acquired. Streptococcus pneumoniae is the most common cause of CAP.
Hospital and Healthcare-Acquired Pneumonia I always caution patients that pneumonia caught during a hospital stay (HAP) or in a long-term care facility (HCAP) can be much more serious. The bacteria in these settings are often more resistant to antibiotics, and the individuals affected are already dealing with other health issues. If you are on a breathing machine, it is specifically called ventilator-associated pneumonia (VAP), which carries a higher risk because it bypasses the body’s natural filtering defenses.
Aspiration Pneumonia Aspiration pneumonia is a unique cause that occurs when you accidentally inhale food, drink, saliva, or vomit into your lungs. I have seen this most often in individuals with conditions that affect their ability to swallow, such as a stroke or Parkinson’s disease. When these substances enter the air sacs, they can cause an infection or chemical inflammation.
For more information on recognizing these issues in your household, I recommend reading our parents guide to pneumonia symptoms.

Who is Most at Risk? Vulnerability Factors
I believe that knowing your risk level is a crucial part of prevention. While pneumonia can affect anyone, I have observed that certain groups face a significantly higher risk of developing a serious infection.
Age-Related Risks The two ends of the age spectrum are the most vulnerable. Babies and children aged two or younger are at high risk because their immune systems are still developing. Conversely, adults aged 65 or older are at risk because immune systems generally weaken with age and older adults often have other chronic health conditions.
Chronic Health Conditions If you are living with certain long-term health problems, your lungs may be more susceptible to infection. I have seen that asthma, COPD, and cystic fibrosis are major risk factors. Heart disease, diabetes, and kidney disease also make it much harder for your body to fight off the causes of pneumonia.
Weakened Immune Systems I have worked with many individuals who have suppressed immune systems due to chemotherapy, organ transplants, or HIV/AIDS. Long-term use of steroid medications can also dampen your immune response, leaving you more open to bacterial and viral invaders.
Lifestyle and Environmental Factors Smoking is one of the most significant lifestyle causes of pneumonia vulnerability because it damages the cilia—the tiny hairs in your lungs that sweep out mucus and germs. I also tell people that living in crowded environments, such as military barracks or nursing homes, increases the likelihood of being exposed to pneumonia-causing pathogens.

The Biological Process: How Your Lungs React
I think it is fascinating—and terrifying—to understand what actually happens inside the lungs during an infection. The primary causes of pneumonia trigger a complex biological chain reaction that leads to the symptoms you recognize.
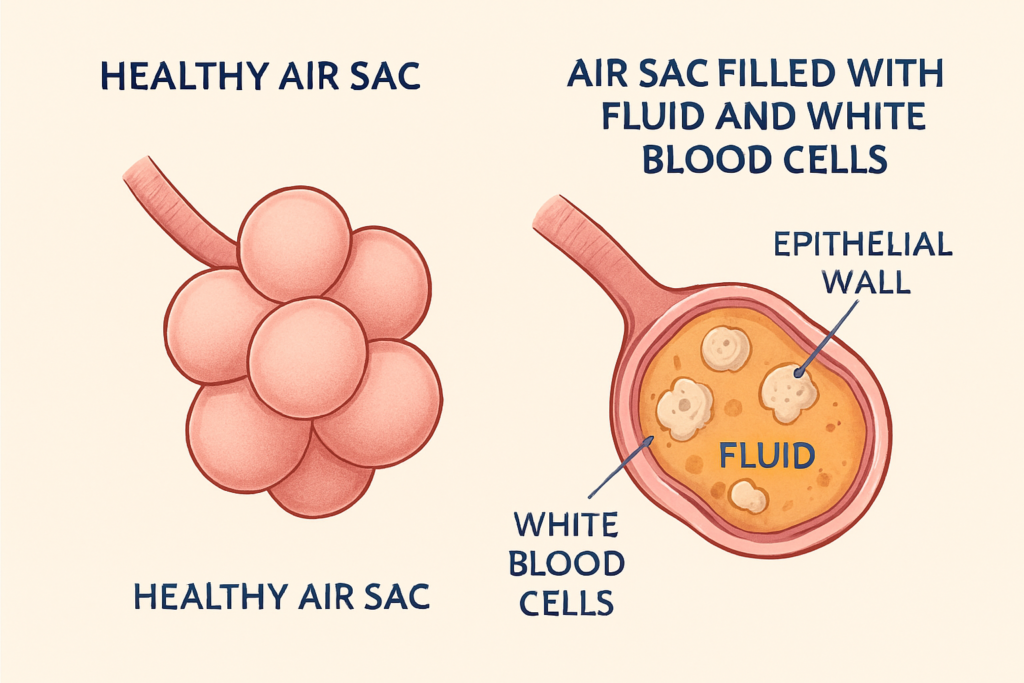
The Inflammatory Response When pathogens enter the air sacs, your immune system sends white blood cells to the area to destroy the invaders. This creates inflammation in the lung tissue. I have seen that this inflammation causes the alveoli to leak fluids, pus, and mucus.
The Problem with Mucus Viscosity The fluid produced during pneumonia is not like simple water. It is often thick, sticky, and highly viscous. I have read that while the poise of water is very low, the “gunk” in your lungs can have a viscosity closer to pudding. This makes it extremely difficult to cough up, especially if the tiny cilia in your airways have been damaged by a previous viral infection.
Consolidation and Airflow In more severe cases, your lung tissue may undergo consolidation. This means the normally spongy, air-filled tissue becomes solid because it is so full of infection and inflammatory byproducts. I want you to imagine trying to breathe through a sponge that has been soaked in honey; that is how some experts describe the feeling of pneumonia.
If you are currently managing your health or looking to stay ahead of the curve, it is worth checking our guide on flu symptoms 2026 to distinguish between a standard virus and the start of pneumonia.
Debunking the Myths: Cold, Rain, and Humidity
I often hear patients ask if “getting caught in the rain” or “being cold” causes pneumonia. I want to clear up this common misconception. Environmental conditions like rain or cold weather do not directly cause pneumonia; only germs can do that.
How Rain Indirectly Affects Your Health While rain itself doesn’t contain the causes of pneumonia, prolonged exposure to cold and wet conditions can cause significant stress to your body. I have observed that this stress can lead to an increased cortisol response, which dampens your immune system activity. When your defenses are down, the germs you are already exposed to—like the bacteria that live in your nose or throat—can take the opportunity to infect your lungs.
The Role of Humidity and Microbes Some research suggests that rain can disturb microbes and spores in the soil, making them easier to breathe in. If you are already immunocompromised due to the stress of exposure, these airborne droplets might lead to an infection. According to the American Lung Association, identifying the specific pathogen is vital because bacterial infections require different treatments than viral ones.
Beautiful Insight: I always tell my patients that while cold weather doesn’t make you sick, it does change how we interact. We spend more time indoors in poorly ventilated spaces, which increases the transmission of the viruses and bacteria that cause pneumonia.

The Link Between Aspiration and Pneumonia
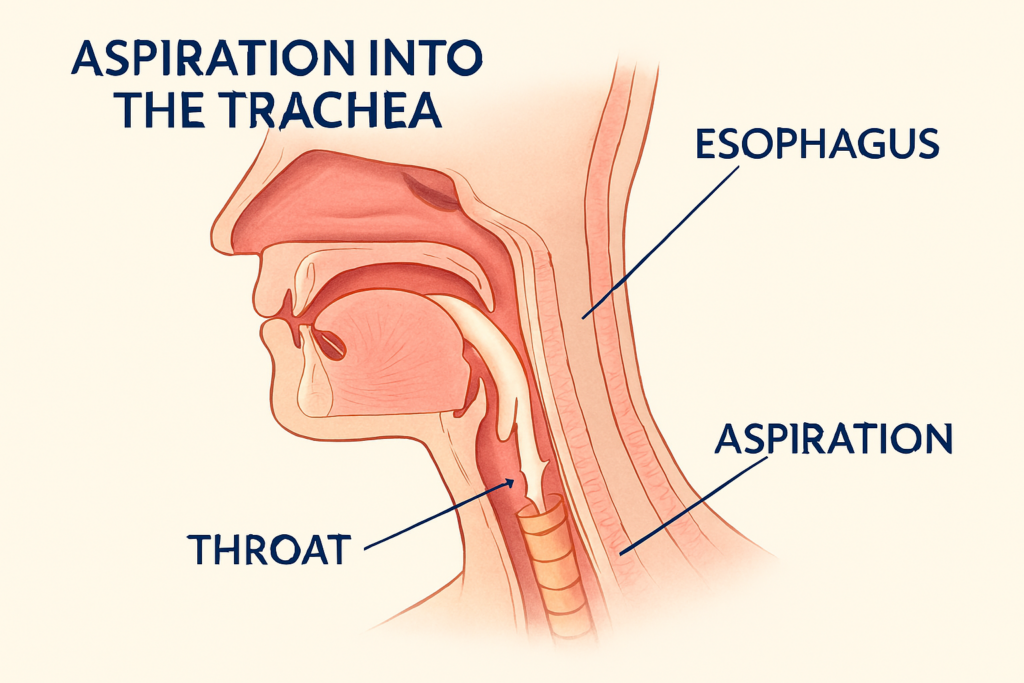
I believe that aspiration pneumonia deserves its own focus because it is often overlooked. This occurs when something besides air enters your windpipe.
The Mechanism of Aspiration Normally, your body has a strong gag reflex and a physical closure of the windpipe when you swallow. However, if that reflex is suppressed—perhaps by alcohol use, drug overdose, or a brain injury—substances like saliva or vomit can trickle into the lungs. I have seen that even “microaspiration,” where tiny amounts of throat secretions enter the lungs over time, is a major cause of pneumonia in the elderly.
Neurological Risks Conditions like dementia or Parkinson’s disease significantly increase this risk. I recommend that caregivers for these individuals pay close attention to any coughing or choking during meals, as these can be early signs of aspiration that may lead to pneumonia.
For those looking to maintain a healthy lifestyle and strong immunity, focusing on overall wellness is key. You might find our healthiest weight loss diet guide helpful for building a body that is resilient against respiratory stressors.
Prevention and Long-Term Lung Health
I am a firm believer that the best defense against the causes of pneumonia is a proactive offense. There are several steps you can take to significantly lower your risk of developing this serious infection.
The Importance of Vaccination Vaccination is your primary tool. I recommend talking to your doctor about pneumococcal vaccines, which protect against several strains of the most common pneumonia-causing bacteria. Keeping up with your annual flu shot and COVID-19 boosters also reduces the risk of the viral infections that often lead to pneumonia.
Hygiene and Lifestyle Habits I cannot stress the importance of handwashing enough. Regularly washing your hands with soap and water is one of the most effective ways to stop the spread of respiratory germs. Furthermore, quitting smoking is essential; I have seen that once you stop smoking, your lungs begin to recover their natural ability to clear out mucus and pathogens.
Building a Strong Immune System I always encourage my patients to focus on the basics: get enough sleep, exercise regularly, and eat a nutrient-dense diet. A healthy body is much better at filtering out the pathogens that cause pneumonia before they have a chance to take hold.
FREQUENTLY ASKED QUESTIONS
Q: Is pneumonia contagious?
A: Pneumonia itself is not contagious, but the bacteria and viruses that cause it certainly are. For example, you can catch the flu from someone else, and that flu can then turn into pneumonia in your own lungs. Fungal pneumonia, however, is not spread from person to person at all.
Q: Can you have pneumonia without a fever?
A: Yes, it is possible. I have observed that older adults, newborns, and people with very weak immune systems might not develop a fever, or they might even have a lower-than-normal body temperature.
Q: How long does it take to recover?
A: Recovery depends on the cause and your overall health. I find that healthy individuals often start feeling better within a few days of starting treatment, but a cough and fatigue can linger for several weeks or even a month.
Q: What is the difference between walking pneumonia and regular pneumonia?
A: Walking pneumonia is a non-medical term for a milder case caused by atypical bacteria like Mycoplasma pneumoniae. It is called “walking” pneumonia because the symptoms are usually not severe enough to require bed rest.
Empowering Your Breath
I hope this guide has helped you understand that the causes of pneumonia are varied and complex, but they are not unavoidable. By recognizing the microbial invaders, understanding your personal risk factors, and debunking common myths about cold weather and rain, you are now better equipped to protect your health and the health of your family.
I encourage you to stay vigilant. If you or a loved one experiences difficulty breathing, persistent high fever, or a deep cough with colored mucus, please seek medical attention immediately. Your lungs are delicate yet remarkably resilient, and with the right knowledge and care, you can help them stay clear and strong for years to come. Take a deep breath and stay healthy!

