I know the heavy, hollow feeling that settles in your chest when you hear your child struggle for breath in the middle of the night. I have stood by a crib, listening to a persistent cough that sounds different than a typical cold—more labored, more exhausting. When a doctor finally says the word “pneumonia,” it feels like the world stops for a moment. You are not alone in that fear; pneumonia is a significant inflammation of the lungs that affects children worldwide, accounting for 14% of all deaths of children under five years old. It occurs when the small air sacs in the lungs, known as alveoli, fill with pus and fluid instead of air. This makes every breath painful and limits the amount of oxygen your child can take in.
While the diagnosis is daunting, I have learned that children possess a remarkable ability to bounce back. As a parent who has navigated the “mama head” spiral of worry, I want to share a comprehensive look at what pneumonia in children really entails. This guide draws on leading pediatric expertise and the real-world experiences of parents who have walked this path, helping you move from panic to empowered action. If you are just starting this journey, I recommend reading this parents guide to pneumonia symptoms and recovery for a high-level overview of what to expect.
Understanding the Basics: What is Happening in Those Little Lungs?
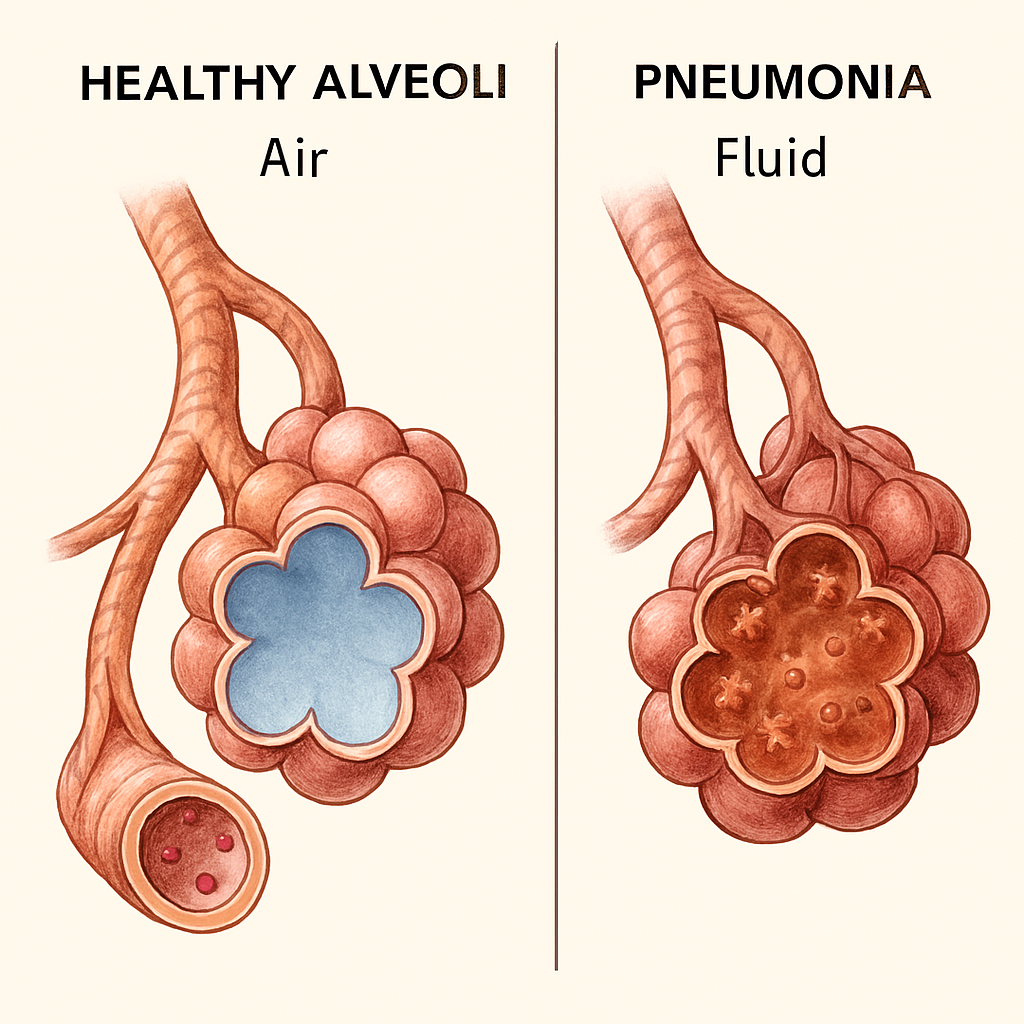
To fight this infection effectively, I first had to understand exactly what was happening inside my child’s lungs. Pneumonia is not a single disease but an acute respiratory infection caused by various agents, including viruses, bacteria, or fungi. In a healthy lung, the alveoli expand with air during inhalation. In a child with pneumonia, these sacs are compromised by inflammatory fluid.
I’ve found that the “where” and “how” of the infection matter to the medical team. Doctors often categorize pneumonia based on how it appears on an X-ray. You might hear the term lobar pneumonia, which means the infection is concentrated in one or more sections (lobes) of the lung. Alternatively, bronchial pneumonia (or bronchopneumonia) appears as patches throughout both lungs. To learn more about the environmental triggers that lead to these conditions, you can explore the different causes of pneumonia.
I have seen how this infection settles in. It often starts as a simple upper respiratory infection before traveling deeper into the lungs. In some cases, a child can even develop pneumonia through the blood, especially during or shortly after birth. Understanding these mechanisms helped me realize that pneumonia in children isn’t just a “bad cold”; it is a systemic challenge that requires targeted intervention.
The Different Faces of Pneumonia: Viral, Bacterial, and Walking
The cause of the infection dictates the treatment, and I’ve learned that misidentifying the type can lead to frustrating delays in recovery.
Viral Pneumonia: The Most Common Culprit Viruses cause most cases of pneumonia in children, with Respiratory Syncytial Virus (RSV) being a frequent culprit for those under five. I’ve noticed that viral pneumonia symptoms often appear more gradually and tend to be milder initially. You might notice wheezing, which is much more common in viral cases than bacterial ones. Because antibiotics do not kill viruses, the treatment for this type is largely supportive—focusing on rest and fluids.
Bacterial Pneumonia: The Sudden Strike Bacterial pneumonia often strikes more suddenly and severely. The most common bacterium involved is Streptococcus pneumoniae. When bacteria are at play, I’ve seen kids develop a sudden high fever, a productive cough, and rapid breathing almost overnight. This type requires antibiotics, such as amoxicillin, to clear the infection.
Mycoplasma or “Walking” Pneumonia This is a unique “atypical” pneumonia that I often see in school-aged children. It’s called walking pneumonia because children may seem surprisingly active and less severely ill despite a persistent, dry cough that can last for three to four weeks. Unlike other types, symptoms usually do not start with a cold; instead, a fever and cough are the first signs to develop.
SECTION INSIGHT: One of the most critical things I’ve learned is that viral pneumonia can make a child susceptible to a bacterial superinfection. If your child seems to be getting better but then suddenly crashes with a high fever (102-103°F) and worsening symptoms, it may mean a secondary bacterial infection has taken hold.

Recognizing the Red Flags: Symptoms You Can’t Ignore
I have learned to look past the general “fussiness” of a sick child and focus on specific clinical signs. While every child experiences symptoms differently, there are hallmark indicators of pneumonia in children that I always monitor.
Respiratory Distress and “Indrawing” The most critical sign I monitor is the work of breathing. For children under five, pneumonia is often diagnosed by the presence of fast breathing or lower chest wall indrawing. This is when the chest moves in or retracts during inhalation, whereas it should expand in a healthy child. If you see your child’s ribs “sucking in” with every breath, this is a sign they are working too hard to get oxygen.
Other Common Symptoms
• Fever and Chills: Often accompanied by sweating or a flushed appearance.
• Persistent Cough: This may be dry or productive, meaning it produces mucus.
• Chest or Belly Pain: I was surprised to learn that pneumonia can cause abdominal pain, which sometimes leads parents to mistake it for a stomach bug.
• Lethargy and Poor Feeding: In babies, I look for a lack of interest in nursing or poor feeding; in older kids, a significant decrease in activity is a major red flag.
• Vomiting or Diarrhea: These gastrointestinal symptoms can often accompany the respiratory struggle.
The Path to Diagnosis: Navigating the Medical System
I’ve had moments where I felt “fobbed off” by a doctor telling me it’s just a “daycare lurgy,” only to find out later it was indeed pneumonia. This taught me the importance of being a persistent advocate. A standard diagnosis usually involves a physical exam where the doctor listens for crackling sounds in the lungs, but further testing is often needed.
Common Diagnostic Tools
- Chest X-ray: This is a primary tool for identifying inflammation in the lung tissue. Interestingly, some cases of pneumonia show a “clear” X-ray early on, only to show infiltrates later as the infection progresses.
- Pulse Oximetry: A painless sensor taped to a finger or toe to measure blood oxygen levels. I’ve seen parents push for more investigation when their child’s levels drop to 96% or lower.
- Blood Tests: A blood count (CBC) can provide evidence of an active infection.
- Sputum Culture: Testing material coughed up to identify the specific pathogen.
If your child has recurring pneumonia—for example, twice in a short period—I suggest asking for a referral to a pediatric pulmonologist. I have learned that repeated infections aren’t always just bad luck; they can sometimes be a sign of underlying issues like asthma or immune system sensitivities.

Home Care Strategies: Supporting Your Child’s Recovery
Most children with pneumonia can recover safely at home with basic care. I focus on creating a “healing sanctuary” where my child’s body can dedicate all its energy to fighting the infection.
Hydration and Nutrition I make it my mission to keep the liquids flowing. Increased fluid intake helps thin out mucus, making it easier for the child to cough up. Whether it’s water, broth, or electrolyte drinks, small sips throughout the day are vital to prevent dehydration.
Comfort Measures
• Cool Mist Humidifier: I keep one running in the bedroom to help soothe the airways.
• Fever Management: Acetaminophen or ibuprofen can help ease discomfort. I never give aspirin to my children or teens due to the risk of Reye syndrome, which can be life-threatening.
• Restful Positioning: For older toddlers, I’ve found that propping them up slightly with pillows or holding them upright can prevent mucus from “pooling” and help reduce nighttime coughing fits.
I also want to mention that you should always ask your doctor before using over-the-counter cough medicines. These are generally not recommended for children under six years old. If the doctor prescribes antibiotics, I make sure to give the medicine on schedule for the full duration, even if my child starts looking better after 24 hours.

When the Hospital is Necessary: Support and Strength
I have read heartbreaking stories of parents sitting in the Pediatric ICU (PICU), watching their children battle severe cases. Hospitalization is recommended for severe cases, especially if a child is having trouble breathing, is dehydrated, or has a persistent high fever.
In a hospital setting, your child may receive: • IV Antibiotics and Fluids: Faster-acting than oral medications, especially if a child is vomiting and cannot keep medicine down. • Oxygen Therapy: To ensure the body gets enough oxygen while the lungs heal. • Frequent Suctioning: To clear thick secretions from the nose and mouth. • Nebulizer Treatments: To help open up the airways if the child is wheezing.
One of the most encouraging things I’ve heard from pediatric nurses is how quickly children can turn a corner. I’ve read accounts of children who were lethargic and on feeding tubes for 48 hours, only to wake up on the third day banging their cup for more juice. Within 36 hours of proper hospital intervention, many children show dramatic improvement.

Building the Shield: Prevention and Protection
I believe that prevention is just as important as the cure. While we cannot avoid every germ, we can significantly lower the risks through proactive measures.
• Immunization: This is the most effective way to prevent pneumonia. I ensure my children are current on vaccines for Hib, pneumococcus, measles, and whooping cough (pertussis). • RSV Tools: New RSV vaccines for pregnant mothers and antibody shots for infants provide a critical layer of protection during RSV season. • Nutrition: Exclusive breastfeeding for the first six months improves a child’s natural defenses. • Environmental Factors: I avoid exposing my children to secondhand smoke and ensure our home has good air quality, as indoor pollution from biomass fuels can increase susceptibility. • Hygiene: Simple handwashing with soap remains a powerful tool for stopping the spread of respiratory germs.

Frequently Asked Questions
Q: Is pneumonia in children contagious? A: Generally, the inflammation of the lungs itself isn’t contagious, but the viruses and bacteria that cause it definitely are. They spread through airborne droplets from coughs or sneezes, or by sharing utensils and cups.
Q: How long does recovery typically take? A: Bacterial pneumonia often clears in 1 to 2 weeks with treatment. However, viral and walking pneumonia can take 4 to 6 weeks for the cough to resolve completely.
Q: What if the first antibiotic doesn’t work? A: I have seen many cases where a child is on amoxicillin but doesn’t improve. This might be because the infection is “atypical” (like walking pneumonia) and requires a different antibiotic like azithromycin. Always check with your doctor if symptoms worsen after 48-72 hours of medication.
Conclusion: A Path to Brighter Days
Watching your child face pneumonia is an emotional marathon. I have learned that the best tools we have are our instincts, our patience, and our willingness to advocate for the best care possible. It is okay to cry in the parking lot, and it is okay to ask the doctor “one more question” until you feel confident in the plan.
The road to recovery might be paved with sleepless nights and humidifiers, but it also leads to that beautiful moment when your child’s energy returns. Our children are resilient, and their bodies are designed to heal. By staying vigilant, supporting their immune systems through nutrition and vaccines, and following medical guidance, you are doing exactly what they need to breathe easy again. Stay strong, keep them hydrated, and know that better, healthier days are just around the corner ❤️.

