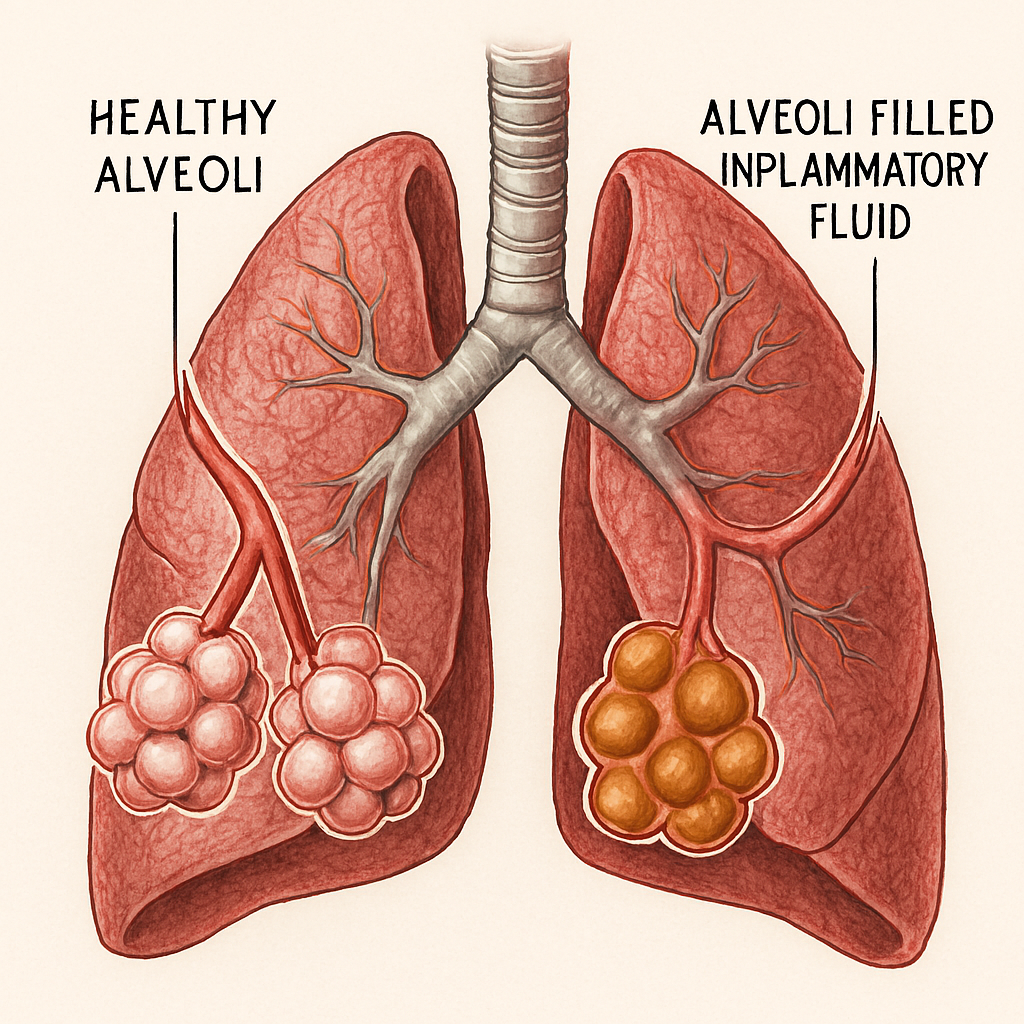
I know that few things are more unsettling than hearing a deep, rattling cough from a child or watching an elderly relative struggle with unexplained confusion and fatigue. In my experience as a health advocate, I have found that understanding pneumonia – symptoms and causes is the most powerful tool a caregiver can possess. Pneumonia is not a single disease but an infection that causes inflammation in the air sacs of one or both lungs. These tiny sacs, known as alveoli, may fill with fluid or pus, which makes it incredibly difficult for oxygen to reach your bloodstream. This guide is designed to help you recognize the signs early, understand the microscopic culprits, and take proactive steps to safeguard your loved ones.

The Biology of Breath and Infection
I find it helpful to visualize the lungs as a complex, upside-down tree. The trunk is the trachea, and the branches are the bronchi, leading finally to the “leaves,” or the alveoli. In a healthy body, these alveoli inflate and deflate easily with every breath. However, when a breakdown in the body’s natural defenses occurs, germs can invade and multiply within the lung tissue.
As the infection takes hold, white blood cells rapidly accumulate to destroy the attacking organisms. This immune response, while necessary, is what leads to the characteristic inflammation of pneumonia. The space between cells and adjacent alveoli becomes filled with neutrophils, bacteria, and fluids leaked from surrounding blood vessels. I have seen how this “consolidation” of fluid impairs oxygen transport, leading to the shortness of breath and fatigue that define the condition.
There are different patterns of this infection. Lobar pneumonia typically affects one or more sections, or lobes, of the lung. Bronchopneumonia, on the other hand, is more scattered and involves the bronchial tubes. Both forms represent a significant challenge to the body’s respiratory efficiency.
I believe that understanding the “why” behind the symptoms can reduce the fear associated with a diagnosis. When you hear the term “fluid in the lungs,” it is simply the physical evidence of your body’s intense battle against an invader.
Decoding Pneumonia – Symptoms and causes by Age Group
In my years of reviewing health information, I have noticed that pneumonia is a “master of disguise.” It does not always look the same in a toddler as it does in a grandparent. The symptoms can range from mild to life-threatening, depending on the germ involved and the person’s overall health.
Classic Symptoms in Adults For most healthy adults, the signs are quite prominent. I recommend watching for:
• Chest pain that worsens when you take a deep breath or cough.
• A persistent cough that may produce thick, yellowish, greenish, or even blood-tinged phlegm.
• Fever, sweating, and shaking chills as the body attempts to fight the infection.
• Shortness of breath during even minor activities.
Atypical Symptoms in the Elderly I want to emphasize that for adults older than 65, the symptoms are often more subtle. Seniors may experience:
• New or worsening confusion or changes in mental awareness, sometimes called delirium.
• A body temperature that is actually lower than normal (hypothermia) instead of a fever. • Increased weakness or unsteadiness, which often leads to falls.
• A loss of appetite and a sudden inability to perform daily activities.
Signs in Newborns and Infants Newborns are the most vulnerable, and they may not show any “classic” signs at all. I urge parents to watch for:
• Restlessness, irritability, or crying more than usual.
• Difficulty feeding or a lack of energy.
• Vomiting or a persistent fever.
• Visible signs of struggling to breathe, such as nostrils flaring or the skin drawing in around the ribs.

The Primary Microscopic Culprits
When we discuss pneumonia – symptoms and causes, we must look at the different microorganisms responsible. I categorize these based on the type of germ: bacteria, viruses, fungi, and parasites.
Bacterial Pneumonia This is often the most severe form. Streptococcus pneumoniae is the most common cause of bacterial pneumonia in the United States. I have noted that it can occur on its own or as a secondary infection after a person has had the flu or a cold. Other bacteria include Staphylococcus aureus, Haemophilus influenzae, and Klebsiella, the latter often seen in alcoholics.
Viral Pneumonia Viruses are the most common cause of pneumonia in children under five years of age. Influenza, respiratory syncytial virus (RSV), and the SARS-CoV-2 virus (which causes COVID-19) are significant triggers. Viral pneumonia is often milder than bacterial, but it can become severe, particularly when it weakens the immune system and allows a secondary bacterial infection to take root.
Fungal and Parasitic Pneumonia Fungal pneumonia is most common in individuals with chronic health problems or weakened immune systems. These fungi are often found in soil or bird droppings. While less common in the developed world, various parasites can also enter the body through the skin or mouth and travel to the lungs, causing significant disruption to oxygen transport.
Where and How Infection is Acquired
I find it useful to classify pneumonia by the environment in which it was contracted, as this often dictates the treatment approach.
Community-Acquired Pneumonia (CAP) This is the most common type and refers to infections caught outside of a hospital or healthcare setting. I know that it affects millions annually and is a leading cause of hospitalization for those over 65.
Hospital-Acquired and Health Care-Acquired Pneumonia Some people catch pneumonia while staying in a hospital for another illness. This form can be much more serious because the bacteria in hospitals may be more resistant to antibiotics, and the patient is already in a weakened state. Health care-acquired pneumonia refers to infections contracted in long-term care facilities or outpatient clinics like dialysis centers.
Aspiration Pneumonia I am often asked about this specific type, which occurs when you inhale food, drink, vomit, or saliva into your lungs. This is more likely if your normal gag reflex is disturbed by brain injury, swallowing problems (dysphagia), or excessive use of alcohol or drugs. Aspiration events can lead to the formation of a lung abscess, which is a pocket of pus within the lung tissue.
Walking Pneumonia “Walking pneumonia” is a non-medical term for atypical pneumonia, often caused by Mycoplasma pneumoniae. I describe this to my readers as a “bad cold” that lingers. It is usually mild enough that you do not require bed rest, but it remains highly contagious through respiratory droplets.
Understanding Risk Factors and Vulnerability
While pneumonia can affect anyone, I have identified several factors that significantly increase a person’s vulnerability.
The Extremes of Age Children age 2 or younger and adults age 65 or older are at the highest risk. In children, their immune systems are still developing; in seniors, the immune system naturally weakens, and they are more likely to have co-existing health conditions.
Chronic Health Conditions I strongly advise those with underlying diseases to be extra vigilant. Conditions like asthma, chronic obstructive pulmonary disease (COPD), cystic fibrosis, and heart disease damage the lungs’ ability to clear out pathogens. Diabetes and malnutrition also impair the body’s general immune response.
Lifestyle and Environmental Factors Smoking is one of the most significant avoidable risk factors. Tobacco smoke damages the lungs’ natural defenses, such as the tiny hairs (cilia) that move mucus and germs out of the airways. Furthermore, living or working in crowded places like nursing homes, dormitories, or military barracks increases the likelihood of exposure to contagious droplets.
I always remind my community that being hospitalized, especially if you require a ventilator to help you breathe, puts you at a much higher risk for developing a severe, antibiotic-resistant form of the infection.
The Path to Diagnosis and Medical Care
If you suspect pneumonia, I believe that seeking early medical attention is non-negotiable. Early detection can prevent the most severe complications.
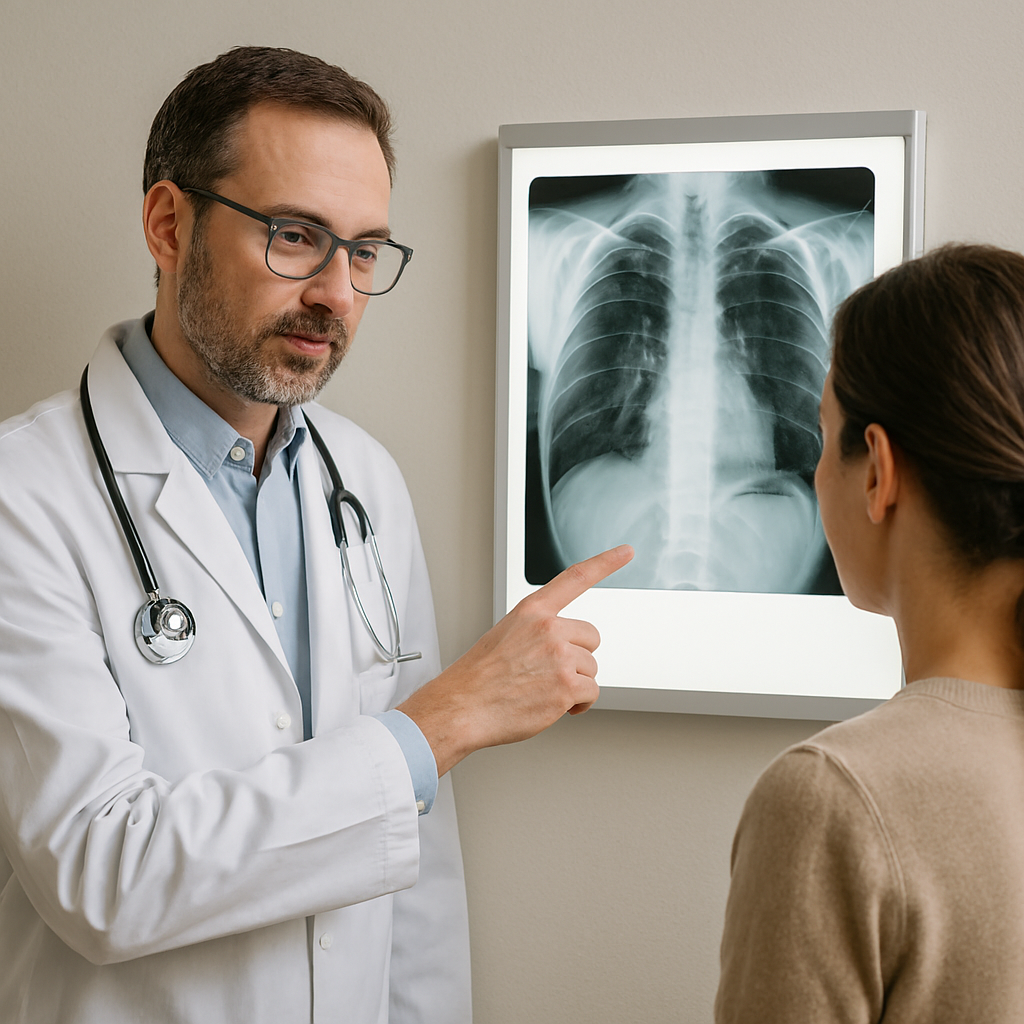
Diagnostic Tools When you visit a healthcare provider, they will likely start with a physical exam, using a stethoscope to listen for crackling or bubbling sounds in your lungs (auscultation). They may also use:
• Chest X-rays: These are essential to see the location and extent of inflammation or fluid in the lungs.
• Pulse Oximetry: A small clip on your finger measures how much oxygen is in your blood. • Blood Tests: These can confirm an infection and help identify if the cause is bacterial or viral.
• Sputum Culture: A sample of your cough’s phlegm can sometimes pinpoint the exact germ responsible.
Treatment Options I have found that treatment depends entirely on the cause. Bacterial pneumonia requires a full course of antibiotics. I must stress the importance of finishing all your medication, even if you start feeling better after a few days, to prevent the infection from returning.
Viral pneumonia cannot be treated with antibiotics. Instead, treatment focuses on supportive care: rest, staying hydrated to thin out mucus, and using fever-reducing medications like acetaminophen or ibuprofen. For some viruses, like the flu, specific antiviral medications may be prescribed if caught early.
Proactive Prevention and Long-Term Lung Health
I am a firm believer that prevention is the best medicine. You can take several concrete steps to reduce the risk for yourself and your family.
The Power of Vaccination I recommend following the official CDC guidelines for vaccinations. Vaccines are available to prevent several types of pneumonia, as well as the flu, COVID-19, and RSV. The pneumococcal vaccine is especially important for children under 2 and adults over 65.
Hygiene and Lifestyle Simple habits make a world of difference. Regular hand washing or using alcohol-based hand sanitizer can stop germs before they reach your respiratory system. I also advocate for:
• Smoking Cessation: Quitting smoking helps restore your lungs’ natural cleaning mechanisms.
• Oral Hygiene: Poor oral health is linked to a higher risk of aspiration pneumonia because bacteria from the mouth can be inhaled into the lungs.
• Immune Support: Focus on a nutrient-dense diet, regular exercise, and getting enough sleep to keep your immune defenses strong.

Potential Complications to Monitor
Even with treatment, I want you to be aware that pneumonia can lead to serious issues, particularly in high-risk groups.
Bacteremia and Sepsis Bacteria can enter the bloodstream from your lungs and spread the infection to other organs, potentially leading to organ failure or life-threatening sepsis.
Pleural Effusion and Empyema Pneumonia can cause fluid to build up in the thin space between the layers of tissue that line the lungs and chest cavity (the pleura). If this fluid becomes infected (empyema), it may need to be drained with a chest tube or surgery.
Respiratory Failure If the infection is severe, the lungs may struggle to get enough oxygen into the blood or clear out carbon dioxide. In these cases, I have seen that patients may require a ventilator or other breathing machines while their lungs heal.
FREQUENTLY ASKED QUESTIONS
Q: How can I tell the difference between walking pneumonia and a regular cold?
A: While both involve a cough and fatigue, walking pneumonia symptoms typically last longer and may include a low-grade fever and chest discomfort. A cold usually stays in the nose and throat, while walking pneumonia affects the lung tissue itself.
Q: Is pneumonia contagious?
A: The microorganisms that cause many types of pneumonia, such as the flu or certain bacteria, are contagious and spread through respiratory droplets. However, aspiration pneumonia is generally not contagious because it is caused by inhaling foreign material into the lungs.
Q: Can you get pneumonia more than once?
A: Yes. Because pneumonia can be caused by many different types of bacteria, viruses, and fungi, having it once does not make you immune to other forms. This is why I emphasize staying up-to-date with your annual flu and pneumonia vaccinations.
Q: How long does the recovery process usually take?
A: Recovery varies. Many people feel better within a week, but a cough can persist for several weeks or even months. For the elderly or those with chronic conditions, full recovery can take much longer and requires diligent rest and nutrition.
Taking Control of Your Breath
Understanding pneumonia – symptoms and causes is more than just a medical necessity; it is an act of love for your family. I have witnessed how quickly a respiratory infection can change from a minor annoyance to a serious health crisis. By learning the specific signs for each age group, from the subtle confusion in a senior to the rapid breathing in an infant, you are positioning yourself as a vital first line of defense.
I encourage you to use the information in this guide not to spark fear, but to inspire action. Focus on the things you can control: maintain excellent hygiene, prioritize nutrient-dense foods, and speak with your doctor about the right vaccination schedule for your household. Your lungs are remarkable, resilient organs, and with the right care and awareness, you can protect the breath that sustains you and those you love. Stay vigilant, stay healthy, and never underestimate the power of early intervention.
